Executive Summary
- An online survey to assess risk perceptions, precautionary behaviour and knowledge of Covid-19 vaccines and of the significance of herd immunity was carried out in December 2020 and January 2021, by Universiti Sains Malaysia and Penang Institute.
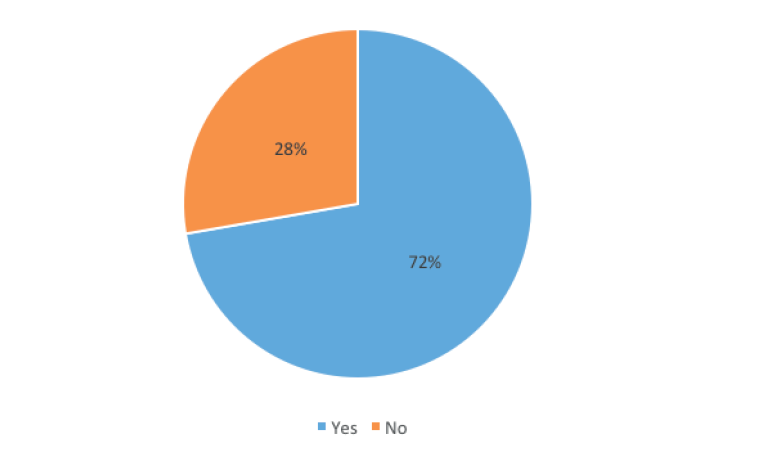
- The study shows that although a majority of respondents (72%) are likely to accept the Covid-19 vaccine, there is still a substantial (28%) proportion of respondents who are not willing to be vaccinated.
- It was also found that the higher the perceived risk is, the lower the vaccination unwillingness will be. Therefore, increasing the population’s consciousness about the seriousness of the disease is vital in improving their willingness to be vaccinated.
- The key barriers to Covid-19 vaccination willingness are a mistrust in the safety of Covid-19 vaccines and concerns about their effectiveness.
Introduction
The long-term success of the public health response to the Covid-19 pandemic will depend on population immunity, also known as herd immunity. However, the proportion of the population that must be vaccinated against Covid-19 to begin inducing herd immunity varies based on the community, the vaccine, the populations prioritised for vaccination, etc.
In order to obtain herd immunity, the government of Malaysia is planning to vaccinate more than 80% of the population, or nearly 27 million people, by the first quarter of 2022 . Its Covid-19 national vaccination plan started in late February 2021. However, immunisation programmes are only successful when there are high rates of acceptance and coverage. Even though Covid-19 vaccine confidence is growing worldwide , vaccine hesitancy and unwillingness remain a big concern.
An online survey was undertaken by Universiti Sains Malaysia and Penang Institute from 1 December 2020 to 25 January 2021 to assess Covid-19-related risk perceptions, knowledge, and precautionary behaviour of Penang’s population, and to describe the current vaccine acceptance landscape in the state of Penang. A total of 411 (with 4.8% Margin of Error) residents from Penang aged 15 and above completed the survey.
Women made up 64% of the study population. The majority of respondents (54.3%) were married, university graduates (70%), and belonging to ages ranged between 25 and 56 years old (73.5%).
A wide range of the respondents (59.1%) were in formal employment; about 15.3% of the respondents were self-employed, and the remainder were from other professions, unemployed, retirees and students (25.5%). Of the respondents in formal employment, 42.4% are professionals working as a doctors, lawyers, engineers, accountants, IT analyst, etc. In terms of monthly household income, the distribution has been quite balanced, with almost one-third in each income group of B40 (32.4%), M40 (36%) and T20 (31.6%) (Appendix: Figure 1-6). Only 1.7% of respondents have had a Covid-19 patient in their family and 29% of them had recovered.
Covid-19-related Knowledge
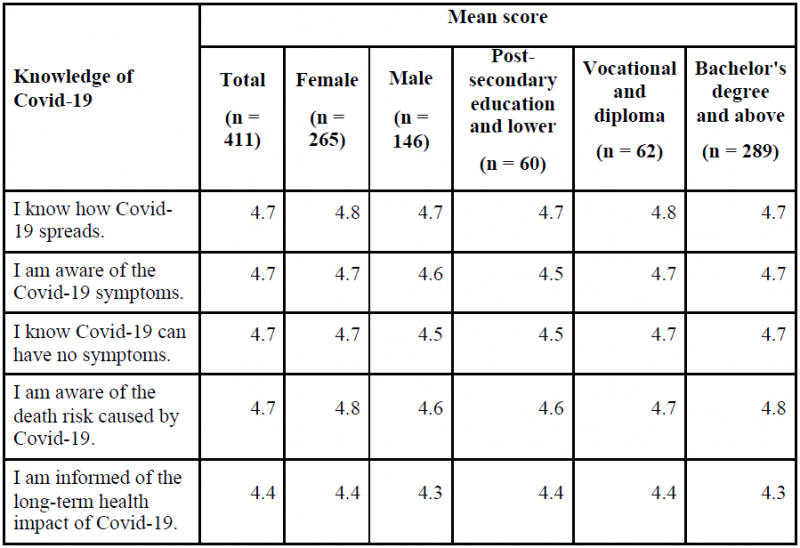
Almost all the survey respondents are aware of Covid-19 symptoms and how it spreads. As many as 96% are aware of asymptomatic Covid-19 infections. Respondents with low education levels reported the lowest levels of knowledge about Covid-19. Moreover, women seem to have a better knowledge about Covid-19 than men (Table 1).
Table 1: Mean scores of Covid-19 knowledge by gender and education level
Perceived risk and precautionary behaviour
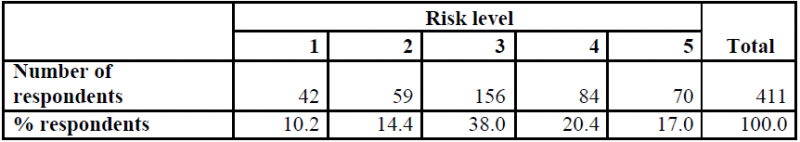
Risk perception is an important factor affecting the public’s willingness to engage in health protective behaviour. Protective behaviour in turn plays a crucial role in controlling Covid-19. In general, the respondents have moderate perceptions of susceptibility. About 37.5% of them agree that there is a high chance of getting Covid-19, while nearly 25% do not believe that the risk of them contracting the virus is high. The average score obtained by the whole sample is 3.2, which corresponds to neither agree nor disagree (Table 2).
Furthermore, about 22.6% of respondents believe that the likelihood of them acquiring and dying from Covid-19 is high, while 36% state that the risk of them dying from Covid-19 is low.
Knowledge of the disease clearly influences risk perception, and those with higher knowledge scores of Covid-19 have a higher risk perception. The risk perception of those who have had Covid-19 patients in their family is higher than those who do not. Surprisingly, younger adults (less than 45 years old) perceive lower risks of getting Covid-19 but greater risks of Covid-19 death than older adults, although scientific evidence shows Covid-19 deaths to be higher among older adults.
Table 2: The perception of the risk level for contracting Covid-19
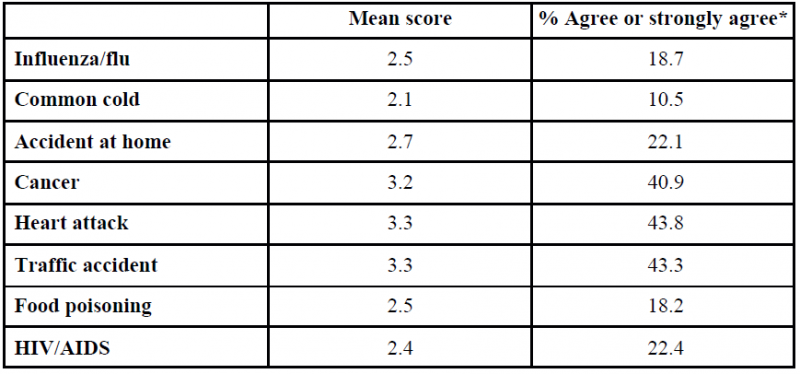
To compare Covid-19-related risk perceptions to other potential threats, respondents were asked to indicate if the risk of them contracting and dying from other disease or accidents is higher than for Covid-19. The majority agree that the risk of them getting infected and dying from Covid-19 is lower than of them getting and dying from cancer, heart attack and traffic accidents, but higher than flu, common cold, accident at home, food poisoning and HIV/AIDS (Table 3). This understanding is more pronounced among men and older adults.
Table 3: Perceived risk of death from other diseases or accidents compared to Covid-19
Respondents were asked whether they feel that they are able to avoid contracting Covid-19 and which actions they have taken to avoid getting it. About 93.2% of respondents believe that they can avoid contracting Covid-19 with proper precautions. Results show that a great majority of respondents always or often wear masks (97.8%), practise social distancing (96.6%), wash hands (94.6%), use sanitisers (92.9%), and avoid large gatherings (92.2%). 83.7% of participants avoid travelling, while 70.1% and 61.6% avoid eating at food hawkers and restaurants, respectively. Meanwhile, 82.5% eat a balanced diet, 64.2% take vitamins and supplements, and 71% exercise regularly. About 56.7% of employed people work from home, more than half of whom are managers or professionals (Appendix: Figure 7). Results indicate that men are less likely to take preventive measures than women. Moreover, respondents with higher education levels, higher age and higher household incomes report the highest levels of preventive behaviour. Better awareness and knowledge about Covid-19 are clearly linked to higher involvement in precautionary behaviour.
Vaccine acceptance
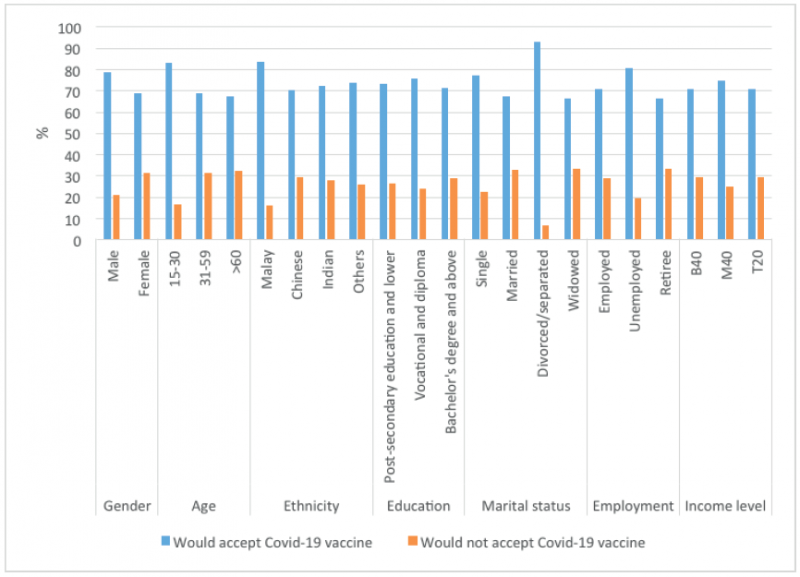
Of the 411 participants surveyed, 297 (72%) say they intend to receive the Covid-19 vaccine; the remaining 28% (114 of respondents) are unwilling. The vaccine acceptance rates differ by socio-demographic characteristics: male (78.8%) to females (68.7%), youth (15-30 year; 83.3%) to older adults (31-59 year; 68.8% and ≥60; 67.4%), Malays (83.7%) to other ethnic groups (just above 70%), and people with less than a college degree (74.6%) to college and/or graduate degree holders (71.3%). High-skilled and white-collar workers (71.1%) are less likely to accept the vaccine compared to blue-collar and service workers (74.3%), and individuals with a higher income (86%) are more likely to refuse the vaccine than those with a lower income (Figure 1 and 2). The mean risk perception score of those who will accept the vaccine is slightly higher (3.2) than those who will not (3.1).
Figure 1: Acceptance of Covid-19 vaccination among Penangites
Number of respondents (N) = 411
Figure 2: Covid-19 vaccine acceptance rate in Penang by socio-demographic categories
(N = 411)
Socio-demographic factors affecting vaccine acceptance
To assess the associations (odds ratios) of socio-demographic factors with Covid-19 vaccine acceptance, a logistic regression analysis is applied (Appendix: Table 1). The regression results show that willingness to accept vaccination is significantly associated with age, gender and marital status. With every one-unit increase in age, the likelihood of accepting a vaccine decreases by about 2%. In other words, the acceptance of Covid-19 vaccines is higher among the youngest individuals, especially those aged 15–30 years, although they are the ones least likely to be affected by the health consequences of Covid-19. This high acceptability in young people may be due to certain social and mental health factors—consequences that are likely to be most pronounced in this age group. A survey conducted by the Research for Social Advancement (REFSA) on the socio-economic impact of Covid-19 on youths in Malaysia shows that youths are one of the groups hardest hit by the Covid-19 crisis. They are often the most vulnerable to economic turbulence, since most of them, especially the youngest among them, are less established in their career. Vaccination can therefore be a source of hope for them, evoking the possibility of a return to normal life.
Covid-19 vaccine acceptance significantly differs based on gender as well. Results reveal that males are 1.7 times more likely to accept Covid-19 vaccines than women. Looking at respondents’ risk perceptions, men (24%) see themselves more at risk of getting infected and dying from Covid-19 than women (22%). Covid-19 mortality statistics from the Ministry of Health Malaysia show that 66.5% of those who died in 2020 were men . Both higher rates of comorbid conditions (e.g. high blood pressure, heart disease, high cholesterol levels and lung disease) and behavioural risk factors (e.g. smoking and drinking) place men at greater risk of death as a result of Covid-19 . Hence, men possibly see themselves more affected and are more keen to take the vaccines compared to women. In addition, the study finds that a majority of women (73.5%) who are not willing to get vaccinated are in their reproductive age . Some of them may be pregnant or considering pregnancy, and misinformation that circulating, especially online, about Covid-19 vaccines and fertility may be putting some women off vaccination. Thus, concerns over fertility and pregnancy may be one of the major drivers of vaccination unwillingness among women, despite explicit reassurances from doctors and scientists.
Additionally, lower vaccination intention among married respondents was also observed. Results reveal that those who are married are 40% less likely to accept the vaccine compared to singles. A majority of them want to wait and see if the vaccines are safe and effective. This is more pronounced among married women. Besides the above-mentioned reasons, family responsibility can also be an important factor that encourages vaccine hesitancy/rejection in married persons.
Although socioeconomic factors are not statistically significant factors influencing vaccination acceptance, recognition of these factors can help develop targeted awareness campaigns directed to the population to increase the vaccination rate.
The study finds that the higher the perceived risk is, the lower the vaccination unwillingness will be. Therefore, increasing the population’s consciousness about the seriousness of the disease is vital in improving their willingness to be vaccinated.
Reasons for refusing the Covid-19 vaccine
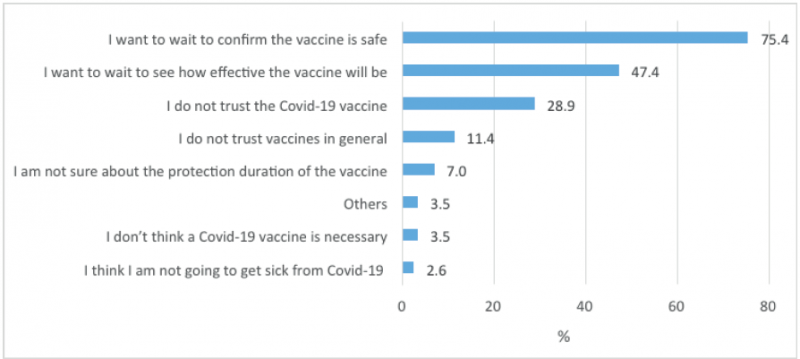
Concerns about vaccine safety (75.5%) and effectiveness (47.4%) are the most common reasons behind refusal of Covid-19 vaccination among the participants (Figure 3). In fact, the vast majority of those who intend to refuse the vaccine want to wait and see how the vaccine is working for other people before getting vaccinated themselves. Nearly 30% express mistrust of Covid-19 vaccines, whilst 11.4% do not trust vaccines in general. About 7% are not sure about the duration of the protection provided by the vaccines. Those in the “wait and see” group are important targets for outreach and messaging, as they express some hesitancy about getting vaccinated, and it may be easier to convince them to accept the vaccine than those who do not trust the vaccine or who are not convinced of the actual need for vaccination.
Despite the remarkable amount of studies carried out since the virus was first characterised, there are still a large number of unknowns about this disease. Concerns about vaccine safety, vaccine effectiveness and protection duration may be due to insufficient data, especially on important population such as children, adolescents, pregnant women and immunocompromised individuals. Over time, data should better clarify what kind of protection the Covid-19 vaccines can induce as well as the effectiveness and duration of the induced protection and help increase confidence and trust in the vaccines.
Figure 3: Reasons for not accepting the Covid-19 vaccine (N = 114)
Measures to improve vaccine up-take
The acceptance or rejection of vaccination by the population will significantly affect the possibility of achieving herd immunity goals and therefore the managing of the Covid-19 pandemic in the long-term. Vaccine rejection is seen when there are concerns over efficacy and safety. Hence, public confidence in the Covid-19 vaccine is important to increase vaccination acceptance rates. Low confidence in the vaccine is reflective of trust, understandings of risk and how immunisation works, and is the result of influence by information being spread through multiple media channels.
There is an urgent need to counter misinformation and provide accurate and reliable information. Educating people about Covid-19 vaccines and how they are developed and monitored for safety can be an effective strategy to help build Covid-19 vaccine confidence. Responsibility for public health education and messaging on Covid-19 vaccines mainly lie with the government, scientists, healthcare professionals and health officials. Engaging with all levels of society as well as targeted evidence-based community messaging are required to combat misinformation on Covid-19 vaccines. Moreover, knowledge about the socio-demographic and psychological profiles of vaccine hesitant/resistant individuals, together with knowledge of what information sources they access, and whom they trust most, can help the government and public health officials develop a proper strategy and efficiently deliver public health messages.
Furthermore, interventions involving online platforms that provide corrective factual information on vaccines and training programmes for community leaders who already have the trust of members of the public (e.g., religious leaders and community groups) to advocate vaccination can help correct misinformation and improve vaccine up-take. In addition, encouraging leaders in the family and in the community or in organisations to be vaccine champions can also increase trust in vaccines.
Building an enabling environment and using open communication to discuss people’s views and uncertainties should help increase vaccine acceptance. Strategies to build vaccine literacy and acceptance should directly address community-specific concerns or misconceptions, and address issues breeding distrust.
For list of references and appendix, kindly download the document to view.
Editor: Ooi Kee Beng
Editorial Team: Sheryl Teoh, Alexander Fernandez and Nur Fitriah (Designer)
You might also like:
![Policymaking and Implementation: Shifting from Hierarchies to Interdependent Polycentric Networks]()
Policymaking and Implementation: Shifting from Hierarchies to Interdependent Polycentric Networks
![Logging in Ulu Muda Forest Reserve: Is Penang’s Water Security under Threat?]()
Logging in Ulu Muda Forest Reserve: Is Penang’s Water Security under Threat?
![Heritage Tourism in George Town: A Complicated and Always Controversial Issue]()
Heritage Tourism in George Town: A Complicated and Always Controversial Issue
![Urgent Need to Strengthen Malaysia’s Legal Framework Against AI-Driven Scams]()
Urgent Need to Strengthen Malaysia’s Legal Framework Against AI-Driven Scams
![Obesity in Malaysia: Unhealthy Eating is as Harmful as Smoking]()
Obesity in Malaysia: Unhealthy Eating is as Harmful as Smoking